

WeChat Official

Internet Hospital

Online Shopping Mall

Sina Weibo
15 April 2026
Ms. Lü, 70, is passionate about sports and exercise in her daily life. She frequently engages in Tai Chi and square dancing, serving as the cornerstone of her family's health and wellness.
An accidental fall resulted in a femoral neck fracture, prompting her to seek treatment at the Orthopedics Department of Sichuan Taikang Hospital, known for its excellent reputation. Following a thorough preoperative evaluation, our physicians discussed the patient's condition and treatment options with her and her family. She subsequently underwent total hip replacement surgery. Throughout the perioperative period, the patient received comprehensive care and guidance. Post-surgery, she was carefully and attentively supported through her rehabilitation exercises, made a smooth recovery, was discharged, and resumed her daily life.

Image source: Taikang Shared Media Resource Platform
The patient and her family were very satisfied with the treatment provided by our department and expressed their gratitude by calling the "12345" mayor's hotline and our hospital.

Image source: Hotline screenshot
For older adults, preventing falls and managing osteoporosis are top priorities. This includes measures like taking calcium and vitamin D supplements, engaging in balance training, and enhancing the safety of the home environment. If you experience a fall, seek medical attention promptly and don’t dismiss it as “just a sprain.”
A delayed diagnosis and treatment of a femoral neck fracture can greatly increase the complexity and risk involved in managing the condition. "The final fracture in one's life" is not predetermined; this saying serves as a warning of its potential danger. With the use of advanced surgical techniques and swift postoperative rehabilitation, most patients can stand up again, regain their ability to walk, and effectively prevent tragic outcomes.
If you or a family member is experiencing this situation, make sure to have a thorough discussion with a professional orthopedic surgeon to determine the most suitable personalized treatment plan.
Knowledge link:
I. Introduction to femoral neck fracture:
1. Femoral neck fracture: "The last fracture of one's life"
After an elderly individual experiences a femoral neck fracture, prolonged bed rest due to pain can quickly result in a range of life-threatening complications, including pneumonia, deep vein thrombosis in the lower extremities, pressure ulcers, urinary tract infections, **etc.** Therefore, it is often referred to as "the final fracture of one's life."
2、The blood supply to the femoral head primarily depends on the vessels that traverse the femoral neck. Once a femoral neck fracture occurs, these blood vessels
3、are easily severed or damaged, causing the femoral head to become like an "isolated island" without supplies, leading to "avascular necrosis of the femoral head." This is one of the serious complications of a femoral neck fracture, meaning the femoral head will collapse and deform, ultimately leading to the loss of hip joint function.
3. Affected population: It mainly occurs in the elderly, especially elderly women with osteoporosis. For them, the femoral neck is the "weak link" in bone strength, and sometimes a fracture can occur from actions as simple as slipping, sitting down too forcefully, or even without any obvious trauma.
4. Symptoms and signs:
If you or a family member experience the following after a fall, a femoral neck fracture should be highly suspected:
(1) Deep groin pain: This is a common symptom, with the pain worsening when pressure is applied to the groin area.
(2) Difficulty standing or walking right away, or within a few days.
(3) Shortening of the affected limb and external rotation deformity: The injured leg looks shorter than the healthy one, and the toes naturally turn outward.
(4) Limited mobility: Difficulty in actively lifting or bending the hip and knee joints.
5. Diagnosis
(1) X-ray film: This is the preferred examination method, as the vast majority of fractures can be clearly displayed.
(2) CT scan: For complex or hidden fractures, a CT scan can provide more detailed three-dimensional information.
(3) Magnetic resonance imaging (MRI): For cases where no obvious fracture line is seen on the X-ray film, but the patient has severe pain and an "occult fracture" is highly suspected, MRI is the gold standard and can detect bone marrow edema in the early stages of a fracture.
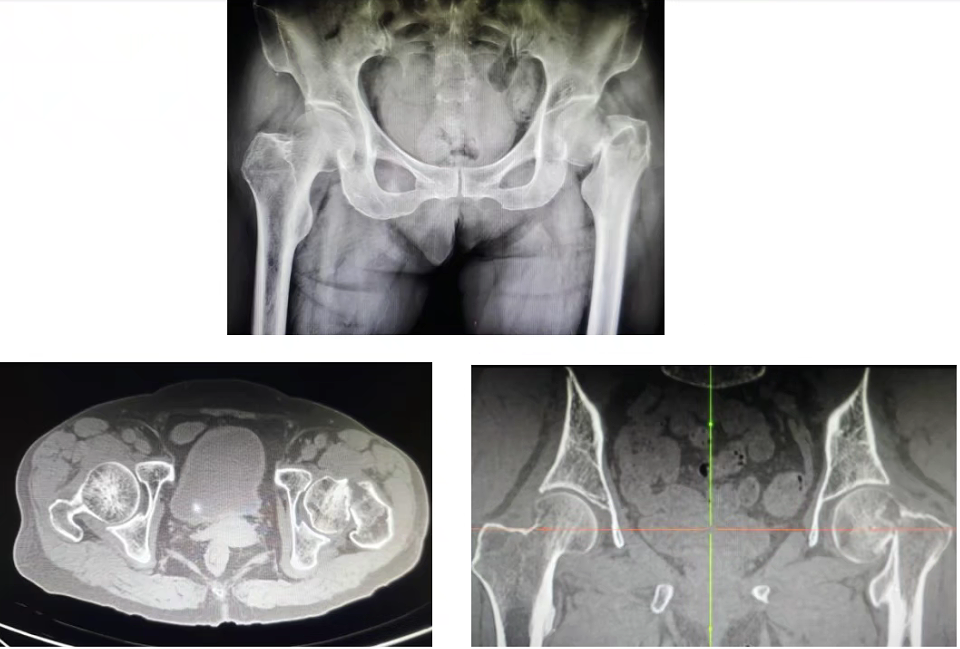
Image source: Department examination image
6. Treatment methods: Depending on age and fracture condition
The treatment decision involves a comprehensive assessment process, with the primary goal of "getting the patient out of bed and moving as soon as possible to prevent complications from prolonged bed rest."
Surgical treatment is recommended as an option: Unless the patient's physical condition is too weak to endure surgery, it is advised to proceed with surgical treatment. For individuals aged 65 and older, hip replacement surgery is considered a preferable choice to mitigate the long-term risk of avascular necrosis of the femoral head and to enable the patient to mobilize and get out of bed sooner.
II. Introduction to artificial hip replacement surgery:
1. Hemiarthroplasty: Only the femoral head part is replaced, preserving the patient's own acetabulum. It is suitable for elderly patients with low activity levels.
2. Total hip arthroplasty: Both the femoral head and the acetabulum are replaced. It is suitable for relatively younger patients with higher activity levels and longer life expectancy. Postoperative functional recovery is better.
3. Lifespan of artificial hip joint prosthesis: With advancements in material science and surgical techniques, modern artificial hip joints have a very long lifespan. Data indicates that more than 90% of artificial hip joints remain functional for 15–20 years, with over 80% lasting beyond 25 years. The lifespan of the prosthesis depends on factors such as the patient's weight, activity level, surgical technique, and the material of the prosthesis itself. Younger, more active patients might have a slightly higher chance of needing a second revision surgery down the line
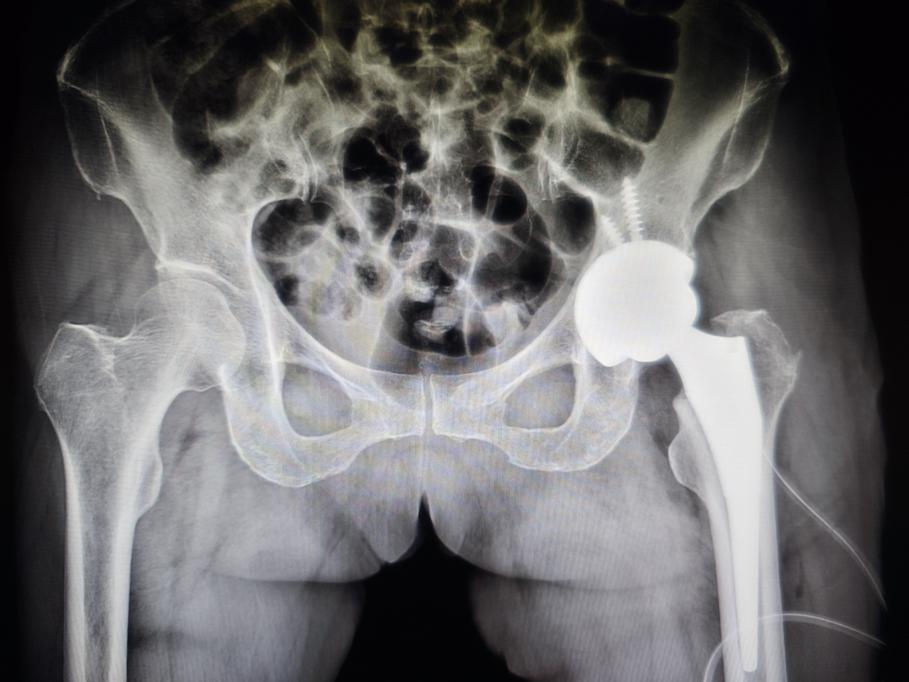
Image source: Department examination image
4. Main indications include:
(1) Osteoarthritis (degenerative arthritis): A common condition caused by the gradual wear and tear of articular cartilage over time, often associated with aging.
(2) Rheumatoid Arthritis: An autoimmune disease characterized by synovial inflammation in the joints, leading to the destruction of cartilage and bone.
(3) Avascular necrosis of the femoral head: This condition arises when the blood supply to the femoral head is disrupted, often due to trauma, excessive alcohol consumption, or hormone use, resulting in its collapse.
(4) Femoral neck fracture: This type of fracture is especially common among the elderly. Undergoing replacement surgery enables them to move around sooner and helps prevent complications associated with prolonged bed rest.
(5) Hip dysplasia: A congenital joint abnormality that can lead to early-onset osteoarthritis in middle age.
5、The goals of the surgery are to relieve pain, improve function, and enhance the quality of life.
6. Important advice for patients
(1) Communicate actively: Fully communicate with your attending physician to understand the pros and cons of the surgery, expected outcomes, and potential risks.
(2) Preoperative preparation: If you smoke, please quit smoking. Control underlying diseases such as hypertension and diabetes. Improve your nutrition and build up your physical strength.
(3) Strictly follow the rehabilitation plan: rehabilitation is the "second surgery," and your effort directly determines the outcome of the surgery.
(4) Remember the anti-dislocation posture (especially for patients with a posterior approach):
* Avoid bending your hip more than 90 degrees.
* Try not to cross your legs.
* Avoid sitting on stools that are too low.
* Avoid internal rotation (adduction) of the affected limb.
(5)Maintain a healthy weight: Managing your weight effectively can greatly increase the lifespan of the prosthesis.
Editor: Li Mingzhu
Reviewer: Li Kainan

